5A: Assessment
This section covers:
- What is a diabetic foot ulcer?
- Risk factors
- Diabetes-related risk factors
- Characteristics
- How to assess
- When to refer diabetic foot ulcers
What is a diabetic foot ulcer?
A diabetic foot ulcer is an ulcer located on the foot and is associated with a loss of protective sensation (neuropathy) and/or a loss of protective sensation and ischaemia in a patient with diabetes.
Diabetic foot ulcers are more likely to occur if the client has uncontrolled or prolonged high blood sugar levels (hyperglycaemia).
IMAGE - M5 01 Diabetic foot ulcerRisk factors
Typical risk factors are outlined in the table below.
| Risk factor | Explanation |
| Hardening or blockages in the arteries (atherosclerosis) | Hardening, narrowing or blockage of the arteries because of fatty deposits (plaques) or cholesterol reduces blood supply to the lower leg. |
| Smoking | Cigarette smoking is a well known risk factor for hardening of the arteries (atherosclerosis) and ischaemic heart disease. |
| High blood pressure (hypertension) | High blood pressure leads to hardening of the arteries. |
| Diabetes | Poorly controlled diabetes leads to high cholesterol levels in the blood and an increased risk of hardening of the arteries. There is also an increased risk of stroke, heart disease and ulceration of the lower limbs. |
| High cholesterol | High cholesterol is a major risk factor for hardening of the arteries. |
| Stress | There is a link between high levels of stress and arterial disease. |
| A history of heart disease, heart attack or stroke | These conditions increase the risk of further problems with the arteries. |
| Obesity | Excess weight, particularly around the waist and thighs, puts extra pressure on the arteries and the heart has to work harder to move blood flow around the body. |
Diabetes-related risk factors
In addition to the risk factors outlined above, there are also a number of diabetes-related risk factors including:
| Risk factor | Explanation |
| Duration of diabetes | The longer a client has diabetes, the higher the risk of developing diabetes-related complications. |
| Unstable blood sugar levels | Poor blood sugar level control leads to an increased risk of diabetes-related complications. |
| Loss of protective sensation | A person with diabetes may have decreased sensation in their feet and are therefore not able to feel if they have sustained an injury to one or both of their feet. |
| Peripheral vascular disease | A person with diabetes is more likely to have arterial disease. |
| Motor neuropathy | Diabetes can lead to muscle wasting and gait changes (i.e. the way a person walks). Often the foot changes shape and may have high arches and clawed toes. Foot deformity and callous formation also results in areas of high pressure in the feet, increasing the risk of ulceration. |
| Autonomic neuropathy | Changes in blood flow to the lower limb results in skin that is drier and more likely to crack. IMAGE - M5 02 Fissures or cracked heels |
| Reduced immune response | There is an increased risk of infection for a person with a diabetic foot ulcer because of impaired blood supply. |
| Previous ulceration | A history of previous foot ulceration is the biggest risk factor for ulceration. If the person has had an ulcer in the past that has altered the structure of the foot, or if they have a joint deformity or previous amputation, this will more than likely lead to an abnormal distribution of pressure on the bottom of the foot and may result in the formation of new ulcers. |
Characteristics
The key characteristics of diabetic foot ulcers are outlined in the following table.
| Characteristics | Diabetic foot ulcer details |
| Wound location | Diabetic foot ulcers usually occur on the sole of the foot, the toes or over pressure points such as the ball of the foot. |
| Wound depth | These types of ulcers are usually shallow but may be deep and may have tracking or undermining (i.e. probes to tendon or bone). IMAGE - M5 03 Deep ulcer on side of foot |
| Appearance of wound bed | The wound bed is usually red or granulating but may also be comprised of black (necrotic) tissue or covered in thick yellow (sloughy) tissue IMAGE - M5 04 Wound bed appearance |
| Wound shape and margins | The wound is usually described as having calloused wound margins. IMAGE - M5 05 Callous surrounding wound |
| Wound leakage (exudate) | Diabetic foot ulcers produce low to heavy amounts of leakage (exudate). An infected ulcer may have purulent, foul smelling leakage. |
| Surrounding skin | The surrounding skin has many characteristics that help us to categorise the leg ulcer as of diabetic origin including:
|
How to assess
Being able to recognise the key signs and symptoms of diabetic foot ulcers is very important to help diagnose a diabetic foot ulcer accurately. There are several important steps that must be performed. These include:
| Step | Explanation |
| 1. Obtain the client’s health history | This includes a history of the present leg ulcer or symptoms. You might like to ask:
It is also important to ask about general medical conditions the person may have, especially heart disease, high blood pressure or cerebrovascular accident, blood sugar levels, eyesight, smoking history, mobility, medication and nutritional status. |
| 2. Examine the client’s legs | Look at the legs and note if there is any swelling. You need to be able to answer these questions:
|
| 3. Examine the client’s foot pulses | You need to palpate foot pulses, particularly the pulse located on top of the foot (known as the “dorsalis pedis pulse”). If this pulse feels weak on palpation (touch), this indicates poor blood flow to the lower limb. |
| 4. Examine the ulcer | Measure the size of the ulcer at least every four weeks or if there is any rapid improvement or deterioration in wound size. This helps to determine if your treatment is working or not.
Note the presence of any smell, the colour of the wound bed, how much exudate or leakage the wound is producing and the condition of surrounding skin. Also, note the characteristics of the wound margin. If the wound margin is calloused, this probably indicates a source of pressure. |
| 5. Measure the Doppler Ankle Brachial Pressure Index (ABPI) | A trained health professional should carry out a hand-held Doppler Ankle Brachial Pressure Index (ABPI) examination. This involves first performing a blood pressure test on both arms and both legs and listening to the arteries with an ultrasound machine, and then comparing the ankle and brachial systolic pressures. This test helps to determine the type of treatment the client may need or if they need to be referred to a specialist for further investigation. |
| 6.Test the client’s sensation using a nylon monofilament | The nylon monofilament test is easy to perform to diagnose clients at risk of foot ulceration because of sensory neuropathy. The test is abnormal if the client can not sense the touch of the monofilament when it is pressed against the foot with just enough pressure to bend the filament. IMAGE - M5 11 Monofilament testing |
When to refer diabetic foot ulcers?
It is very important that you refer your client to a specialist when:
- There is uncertainty in diagnosis (i.e. it is difficult to determine the type of ulcer based on clinical signs and symptoms alone)
- There is a low or high Ankle Brachial Pressure Index (ABPI) (i.e. less than 0.9 or greater than 1.2)
- The client would benefit from surgical revascularisation
- There are signs of infection or inflammation
- There is no progress in wound healing within two weeks of commencing pressure off-loading therapy and debridement (removal) of unhealthy tissue in the wound
- The wound can be probed to bone
- The wound deteriorates and a new ulcer occurs
- The ulcer or lower limb appears ischaemic.
Top of page
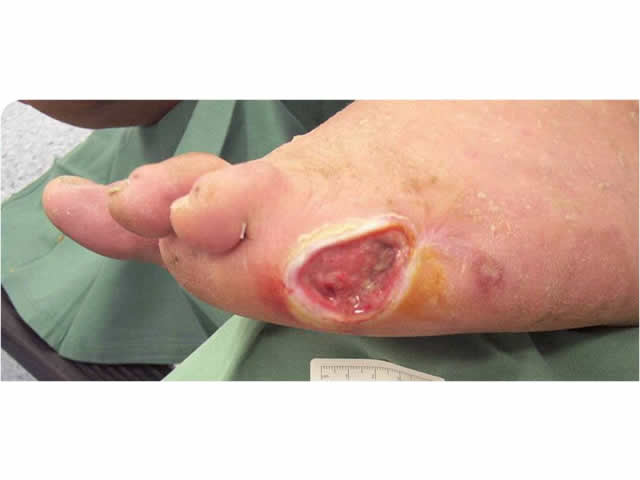
M5 01 Diabetic foot ulcer
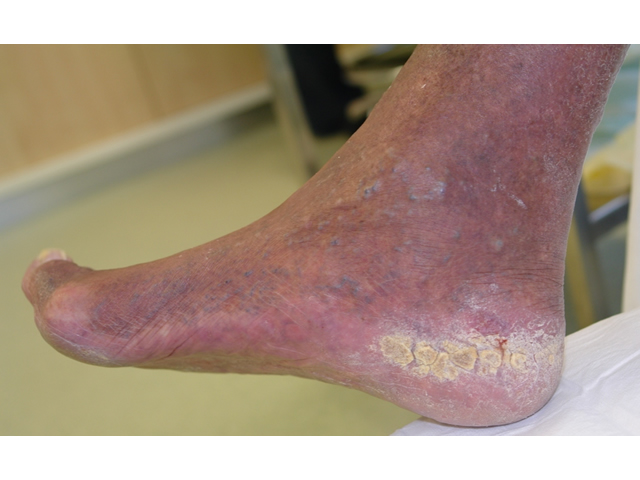
M5 02 Fissures or cracked heels
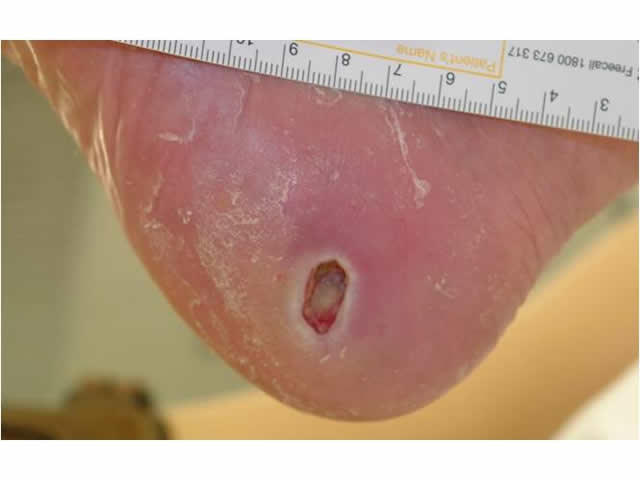
M5 03 Deep ulcer on side of foot
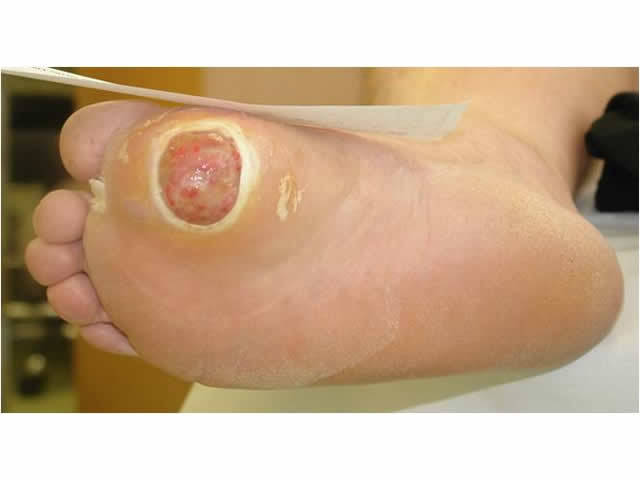
M5 04 Wound bed appearance
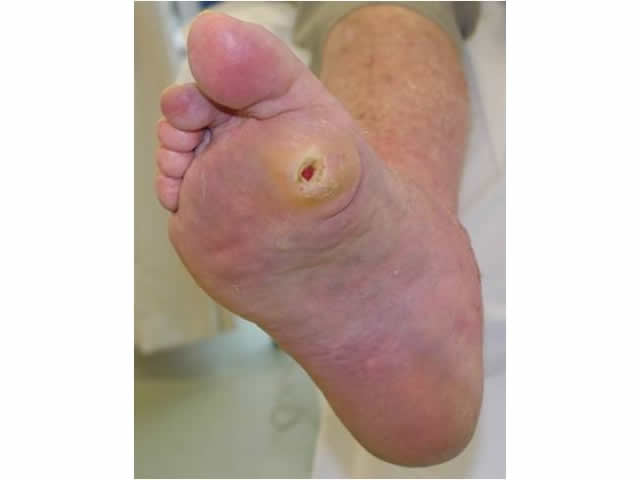
M5 05 Callous surrounding wound
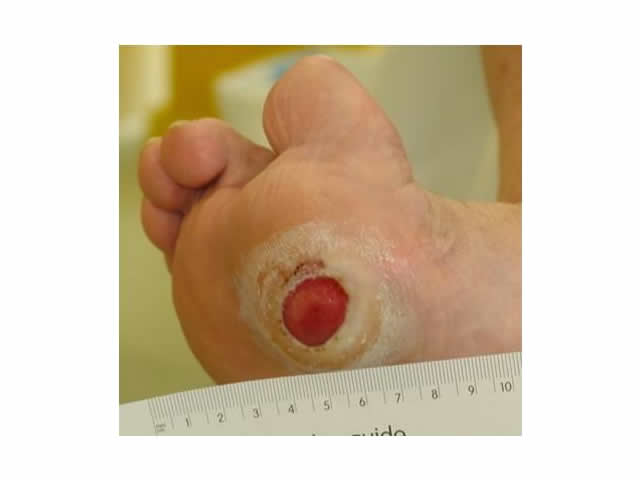
M5 06 Callous surrounding wound
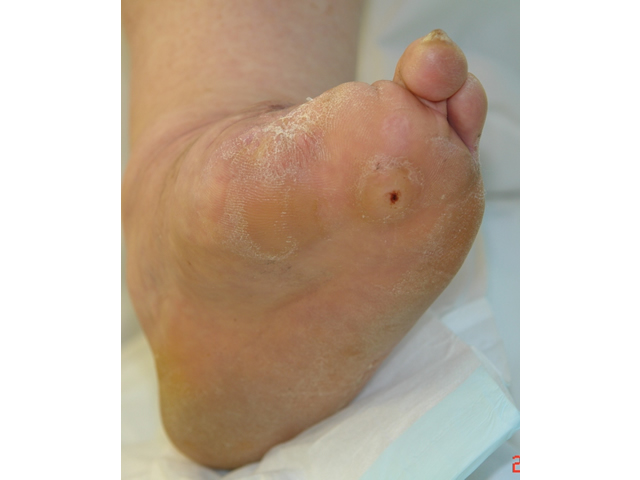
M5 07 Previous amputation
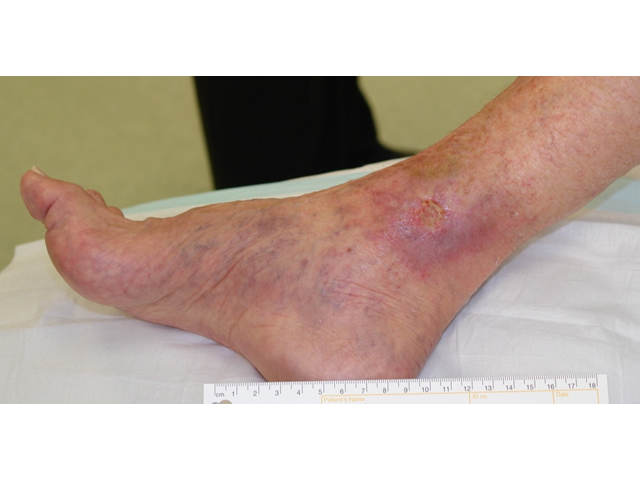
M5 08 Clawed toes
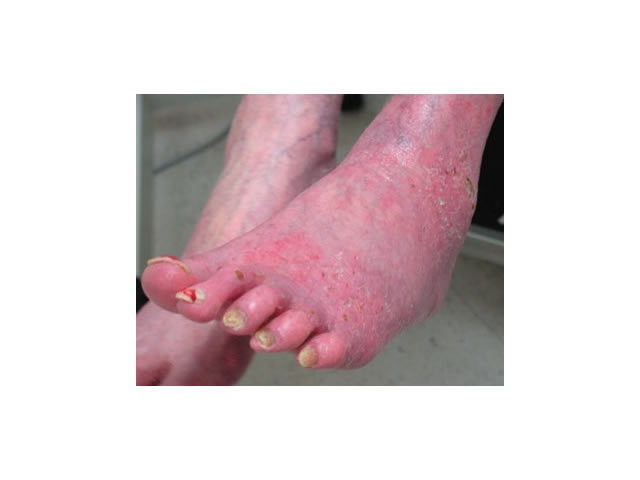
M5 09 Redness in dependent position
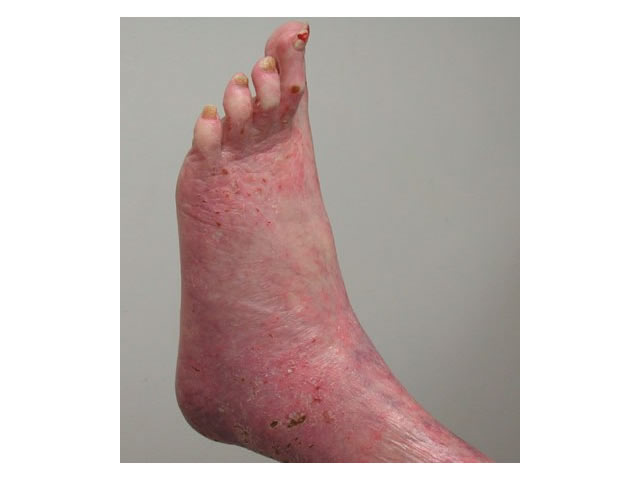
M5 10 Pallor on elevation of leg
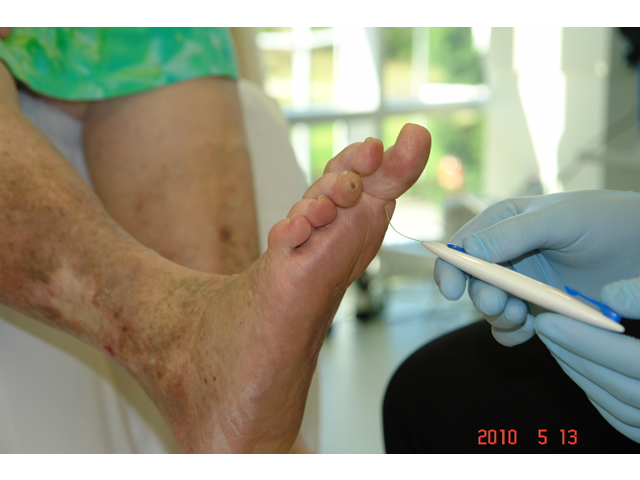
M5 11 Monofilament testing


